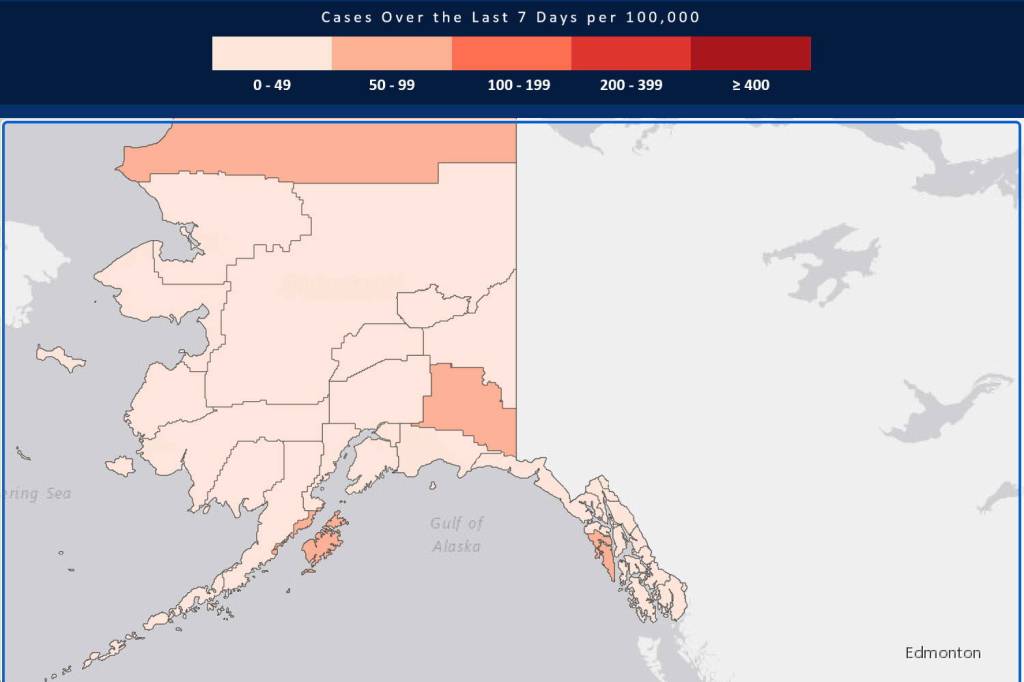
Small uptick in respiratory illnesses, including COVID-19, in Juneau
Published 9:30 pm Tuesday, September 5, 2023


The federally designated Public Health Emergency for COVID-19 may have ended in May, but the disease still lurks, as does the perennial infectious champ, influenza.
And the flu season is just starting.
There was an uptick in the number of flu and COVID-19 cases reported statewide in August, and in Juneau, but there are other science-based tools and measures that provide important insight.
The number of COVID-19 cases among Alaska residents spiked in early August, but came back down toward the end, according to preliminary data from the state’s Department of Health. It is providing COVID-19 and flu numbers for the rest of the summer.
Local numbers are also being watched.
“We saw a slight uptick in our numbers last week, when we had a high of 11 staff out due to illness and two COVID-positive patients,” said Erin Hardin, spokesperson for Bartlett Regional Hospital, which has about 500 employees.
On Wednesday morning there were four hospital staff out with COVID-19 and no patients admitted with COVID-19 or the flu, Hardin said. But within a few hours the total number of hospital staff with COVID-19 had risen to nine people, an example of how quickly things change, said Charlee R. Gribbon, an infection preventionist at Bartlett.
The numbers for employees out with respiratory symptoms had been fairly steady all summer, closer to three to six each week, Gribbon said.
It is important to consider a number of variables connected to hospital employees getting sick relative to the larger population, Gribbon said.
To start, healthcare workers are on the front lines when it comes to exposure to infectious illnesses. Bartlett and other medical centers have strong policies about employees staying home if they experience symptoms, whereas other employers may not object when workers come in sick.
Then there is the educational factor of hospital employees, as a group, recognizing symptoms sooner, Gribbon said.
She focuses more on other measures, like wastewater surveillance.
“Wastewater is an early indicator for me,” said Gribbon. “With that kind of data the trends are more important,” she said. “There are ups and downs, but when there is an increase over two to three weeks it gives me a heads-up.”
Wastewater-based epidemiology is the testing of sewage to provide information on the overall health of a community. Wastewater surveillance isn’t a new science, but it was expanded by the Centers for Disease Control and Prevention (CDC) during COVID-19. Many states, including Alaska, report their numbers, which also contributes to a national outlook.
There are two wastewater collection sites in Juneau that until recently hovered in the mid-600 range, but for the past few weeks are closer to 1,000, Gribbon said. It’s too soon to be alarmed, but not too soon to remind people to be proactive in taking care of themselves and others.
Wastewater surveillance numbers have variables to be considered, too. For instance, the facility downtown would feature samples from tourists in far greater numbers than the one closer to Mendenhall Glacier.
The good news is that as a community, Juneau is well informed and proactive about healthcare overall, Gribbon said.
Data from the Division of Public Health at the Alaska Department of Health shows about 33% of Juneauites received a flu vaccine during the 2022-2023 year, which runs from August to July. That compares to about 23% statewide. Anecdotal observations that more people are wearing masks around town is a very positive sign. Hardin, Gribbon and other medical professionals refer to it as “practicing respiratory etiquette.”
Masks are very effective in limiting exposure, which is the best way to ensure a mild flu season.
“There is plenty of science out there that it reduces our risk,” but it’s also just logical, said Gribbon. “Think about the ways into your body for food, air — and pathogens — it’s mucus membrane. Covering your nose and mouth with a physical barrier blocks access.”
Even the flimsy masks can reduce exposure by 60%. N-95s have that name because they provide 95% protection, she said.
“It isn’t perfect, but it’s much better than nothing,” she said.
Hardin and Gribbon also encourage people to get vaccines for flu, COVID-19, and if 60 years of age or older, RSV, which is respiratory syncytial virus. Flu shots are available now at Bartlett; COVID-19 boosters are due in the next few weeks. RSV is available, but likely to be out of pocket right now.
Gribbon said that getting vaccinated earlier in the season is better, and recommends people get it as soon as it is available to their community. High immunity lasts at least four months, and late January to late March is typically the worst it gets for illness.
“Don’t wait til you get sick,” she said. “Get vaccinated before you get sick.”
• Contact Meredith Jordan at meredith.jordan@juneauempire.com or (907) 615-3190.