Opioid crisis still cuts deep in Alaska
Published 11:00 am Sunday, October 6, 2019








Correction: An earlier version of this story incorrectly reported that the cost of the opioid epidemic to the state of Alaska was $1 billion, according to McDowell Group report. That report referred to the cost of all drug abuse in Alaska, not just opioids. Additionally, the total cost to the state for fiscal years 2017 and 2018 was not over $210 million, it was roughly $193 million. The Empire regrets the errors.
Over a six-year period from 2006-2012, nearly six million prescription pain pills were supplied to the city of Juneau. That’s enough for 27 pills per person, per year. In the entire state of Alaska the number of pills was over 138 million.
On July 16, The Washington Post published a database maintained for years by Drug Enforcement Agency which tracks pain pills throughout the United States. The database, known as the Automation of Reports and Consolidated Orders System, or ARCOS, tracks prescription drug sales throughout the country and provides records from 2006 to 2013.
The DEA had maintained the database for years, but it wasn’t until the Post and other media companies sued the agency under the Freedom of Information Act that the government was forced to make the data public.
The data reveal a stunning amount of prescription opioids flowing to almost every community in the country, even in some of the most rural regions of Alaska. Prescription opioids are widely credited with fueling America’s opioid epidemic, and in the past year, especially in the past several weeks, billions of dollars have been paid out to families, cities, counties and states as pharmaceutical companies begin to take responsibility for their role in America’s massive public health crisis.
The ARCOS data tell us not only how many pills were prescribed, but the manufacturer and the purchaser, along with a number of other data points like dosage and type of drug. It does not tell who the prescribers were or what the pills were prescribed for.
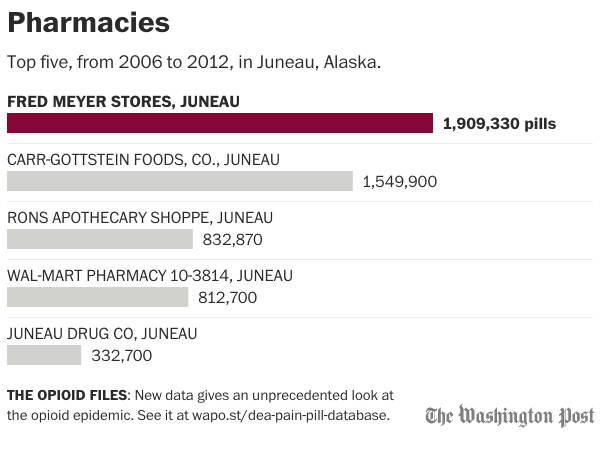
In Juneau, the largest distributor of pills was Fred Meyer, with a total 1,909,330 over six years. Second was Safeway with 1,549,990, and third was Ron’s Apothecary Shoppe with 832,870 pills.
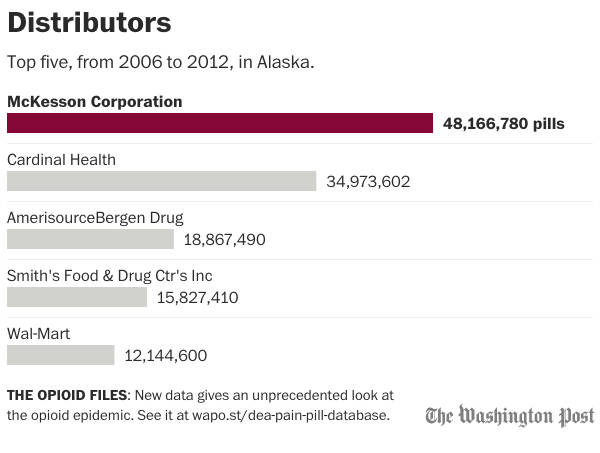
The two largest pharmaceutical companies to sell to pharmacies in Juneau, and in all of Alaska were the McKesson Corporation and Cardinal Health. Far and away the largest manufacturer whose pills ended up in Juneau and Alaska was SpecGx, a subsidiary of Mallinckrodt Pharmaceuticals. According to the Post, the vast majority of pills sold in the U.S. can be traced back to just three companies, Mallinckdrodt being one of them.
The sheer number of pills flowing into the community was the result of over-prescription. Pharmaceutical companies like the recently bankrupt Purdue Pharma spent billions of dollars convincing medical providers that prescription opioids like OxyContin could be prescribed casually, in a manner similar to non-narcotic painkillers like ibuprofen.
In February 2017, then-Gov. Bill Walker issued a disaster declaration in response to the crisis (President Donald Trump declared a national state of emergency in October that same year.) and the state created a number of plans, working groups and programs to address the issue.
In 2016, the Juneau Opioid Workgroup was created. The workgroup is a collection of local health care services and agencies brought together with grant money from the National Council on Alcoholism and Drug Dependence. Among the members of the group are Juneau Alliance for Mental Health Inc. (JAMHI), Southeast Alaska Regional Health Consortium (SEARHC) and the Alaska Division of Public Health. The group works to educate the population about opioids and reduce the number of pills in the hands of the public.
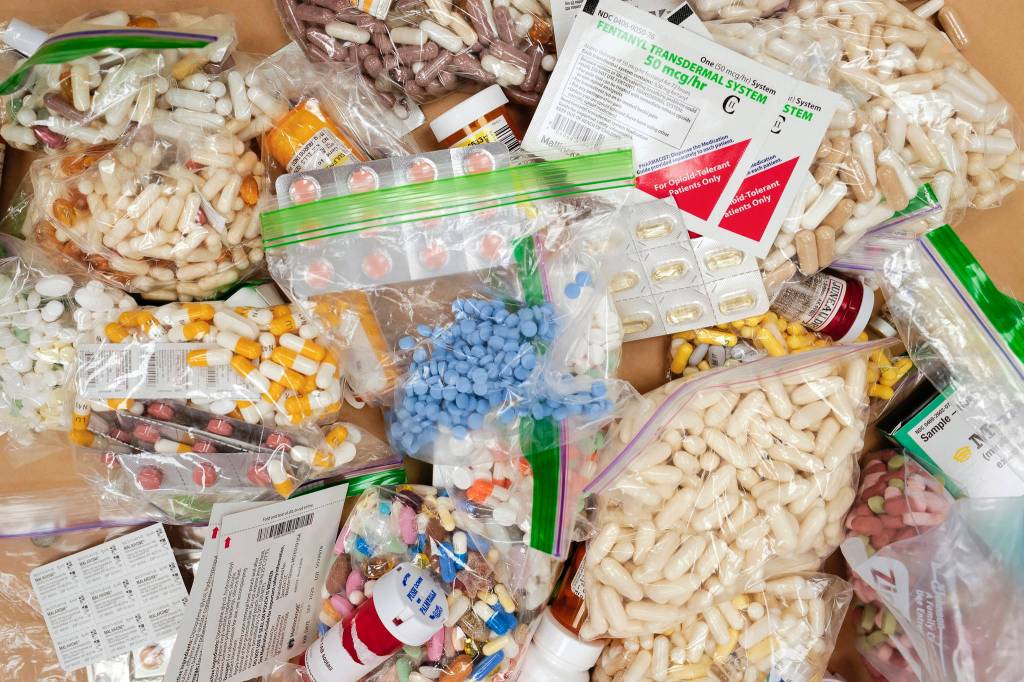
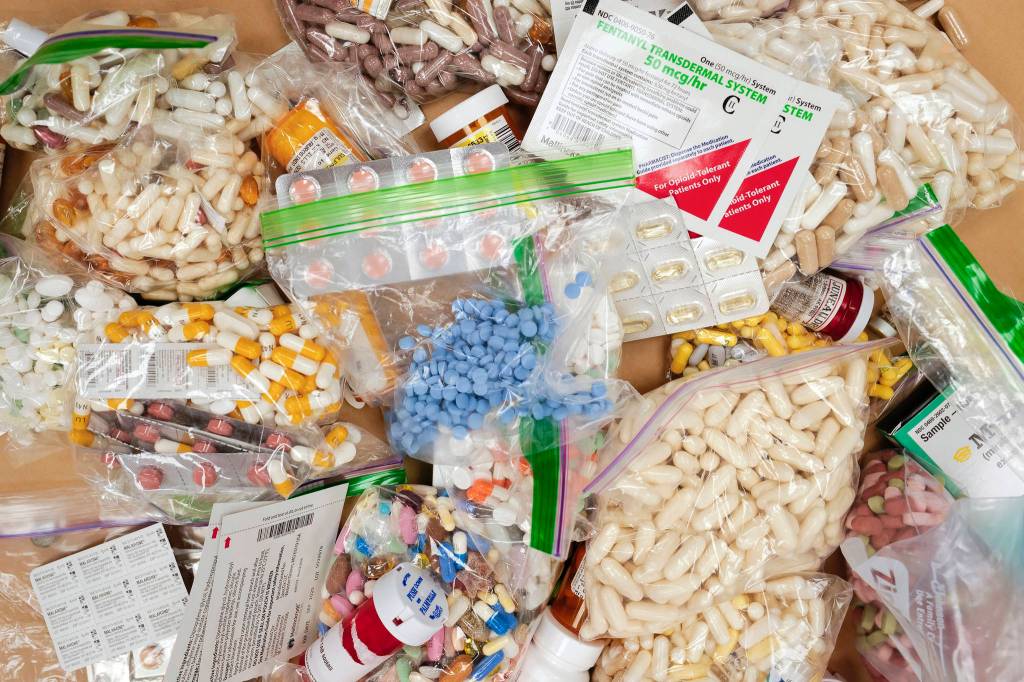
The working group also distributes drug disposal bags to local pharmacies which are given to patients receiving narcotic medication. Patients can put unused pills into the bags and add water to create a chemical solution that destroys the medication. Jessica Spurrier, Partnerships for Success coordinator at JAMHI told the Empire that most pharmacies in Juneau have accepted the disposal bags. However, Fred Meyer, which was the largest distributor of opioid medication has not accepted the bags. Kroger, which owns Fred Meyer, did not respond to a request for comment.
Part of those efforts have focused on working with local pharmacies to distribute educational materials to patients receiving narcotic painkillers along with special disposal bags that can safely destroy leftover medication.
“Things have changed drastically,” said Scott Watts, owner and pharmacist at Ron’s Apothecary. “In general we’ve seen a lot less prescriptions coming in. More visibility on those prescriptions, prescriptions for lower quantities.”
But while the number of prescriptions coming in has gone down, “Eliminating opioids is not an option,” Watts said.
Patients are still using opioids to treat a variety of pain issues. “We’ve got to take care of these people and help them decrease their use and give them other resources.”
Outnumbering alcohol
Data from the Alaska’s Prescription Drug Monitoring Program (PDMP) show that prescriptions for opioids have been declining statewide since 2016 (National Institute of Health data show that Alaska providers wrote 52 opioid prescriptions for every 100 people in 2017). Data from the Department of Health and Social Services show there were 75 deaths from opioid-related overdoses statewide from April 2018 to March 2019, down from the 108 deaths in 2017. None of those deaths occurred in the Southeast region, according to state data. DHSS Communications Director Clinton Bennett told the Empire in an email there had been 18 opioid overdose deaths in Juneau from 2014-2018.
According to state data aggregated from a number of state public health agencies, the cost of the opioid crisis in Alaska for fiscal year 2017-18 was more than $193 million. That amount comes from Medicaid reimbursement, public safety, therapeutic court and other costs. About a third of that, roughly $64 million, is paid for by the federal government but the remainder, more than $129 million, is paid by the state. The Empire previously reported that substance abuse in Alaska was costing the state over $1 billion a year as of 2015. That number comes from a study by the McDowell Group which factored in a number of connected items like loss of productivity and costs borne by the private sector.
But while deaths may be declining overall, Bradley Grigg, Chief Behavioral Health Officer at Bartlett Regional Hospital says he’s seen more people seeking treatment for opioid addiction in the past three years. Grigg oversees Bartlett’s Rainforest Recovery center which offers residential and outpatient treatment programs.
“Three years ago, three out of four patients that we saw at Rainforest, the number one drug of choice was alcohol,” Grigg said. “In calendar year 2018, that three out of four dropped to 50 percent.”
The number of people seeking help from addiction from some form of opiates has been on the rise, Grigg said.
“If the trajectory remains the same over the next two years, we can anticipate that the number of folks entering Rainforest for treatment, opiates would outnumber alcohol.”
A lucrative market
In 2017, the Alaska Legislature passed House Bill 159 which limited the amounts of opioids doctors could prescribe at one time and helped establish the PDMP. But despite efforts to curb prescription opioids, Alaska and Juneau remain lucrative markets for opioids due to their remoteness.
“Alaska has always been a consumer destination,” said Assistant U.S. Attorney Jack Schmidt, who prosecuted drug cases as an Assistant District Attorney for the State of Alaska. “It’s the most lucrative market for any drug, it commands a higher price.”
Schmidt told the Empire that when he was Juneau’s DA in 2010, an ounce of low grade heroin that could be purchased in the Lower 48 for $300-700 could be sold in Juneau for roughly $28,000.
“There’s 28.5 grams in an ounce,” Schmidt said, (the actual number is closer to 28.3) “they were selling it in tenths of a gram. A tenth of a gram would be sold for $100. That’s $1,000 a gram, 28.5 grams in an ounce, that’s $28,500.”
According to data provided to the Empire by the Juneau Police Department, the Drug Enforcement Agency seized over a million dollars in heroin bound for Juneau alone in 2018.
Despite the difficulty in combating drug addiction, gains have been made. There has been an expansion of treatment programs, prevention education efforts and opioid overdose reversal drugs. Juneau Police Department Officers Lt. Jeremy Weske and Sgt. Dominic Branson both credited the drug Narcan, a nasal spray which can be used to reverse an opioid overdose, with saving people’s lives.
“I think that that’s probably credited with saving a bunch of lives,” Branson said in an interview. “We might not even be aware of (how many times they’ve been used) because first responders might not even go to those scenes where someone was revived,” he said.
State data reports that over 7,000 Narcan kits were distributed from August 2017 to July 2018.
All walks of life
Rainforest Recovery has been able to expand both residential and outpatient operations.
“We are serving roughly 400 individuals a year,” Grigg said. “Five years ago we were serving about 75 percent of that.”
Grigg attributes that to Rainforest refining their practice to involve more intense work with shorter lengths of stay.
“The length of stay has been about 23 days, the result of that has been we are serving more patients,” Grigg said. “In our outpatients clinic, a year ago, we had 13 patients, today we have nearly 300. We are seeing a significant boom in the number of patients that are coming through our doors for help, and part of that help is an increase in opiates. It’s kids, adults, adolescents, young adults, teenagers, middle aged, senior citizens.”
Grigg and others who work in fields affected by the opioid crisis have said they believe the widespread impacts of addiction have driven the broad response from the community level all the way to the federal government.
“I think a big contributor is who it’s affecting, and it’s everybody,” Griggs said.
Branson and Weske said they had seen opioid abuse from all walks of life, “it really is pervasive among any age group,” Weske said.
The response to the opioid crisis across the nation and in Juneau has forced a variety of organizations and fields to work towards a common goal. Grigg credits the PDMP with better informing Bartlett’s doctors as to what patients have recently been prescribed. State data from the Department of Commerce show that over a two year period from 2016 to 2018, the number of registered users of the state PDMP rose from more than 1,700 to just over 6,400. In March 2019 there were more than 500,000 patient records requests in the state.
The number of opioid overdose deaths in the state went down from its peak of 104 in 2017 to 64, according to the Division of Public Health. But as the more than $1 million in seized heroin and increased number of people seeking help for opioid addiction show, the crisis remains.
“It’s not going away any time soon with what we’re seeing,” Grigg said. “When you have a town of 33,000, and you’ve got six, seven outfits that are striving to provide service. We’re not competing for patients, we are all working together, we all have patients that come through our door.”
Data
From 2006 to 2012 there were 138,652,246 prescription pain pills supplied to Alaska.
From 2006 to 2012 there were 62,292,963 prescription pain pills, enough for 31 pills per person per year, supplied to Anchorage, Alaska.
From 2006 to 2012 there were 1,706,150 prescription pain pills, enough for 27 pills per person per year, supplied to Sitka, Alaska.
From 2006 to 2012 there were 4,036,622 prescription pain pills, enough for 43 pills per person per year, supplied to Ketchikan Gateway Borough, Alaska.
From 2006 to 2012 there were 397,030 prescription pain pills, enough for 24 pills per person per year, supplied to Haines Borough, Alaska.
From 2006 to 2012 there were 193,900 prescription pain pills, enough for 4 pills per person per year, supplied to Aleutians West Census Area, Alaska.
• Contact reporter Peter Segall at 523-2228 or psegall@juneauempire.com.